Known as one of the largest insurers, Delta Dental is actually composed of 39 independent Delta Dental companies under the Delta Dental Plans Association with one goal in mind: to provide quality oral care for their members (patients) via their contracted providers (Dentists)
During my almost 3 years at Delta, I have been on the Provider Experience team, which has ambitiously set out to implement a global digital adoption strategy for our Providers, particularly through our main application, Provider Tools (PT). Within PT, providers can submit claims, check a member’s eligibility & benefit details, sign up for direct deposit, and more recently, make adjustments on their claims, or dispute a decision made by Delta.
EFT/ERA Signups
My team was involved with enhancing the electronic payment (EFT) and earned remittance advice (ERA) sign up flow. By implementing these changes, which included automatically generating cases in our backend system, Delta Dental was able to improve direct deposit enrollment TATs by 5 business days saving case processing time by 1000s of hours per year.
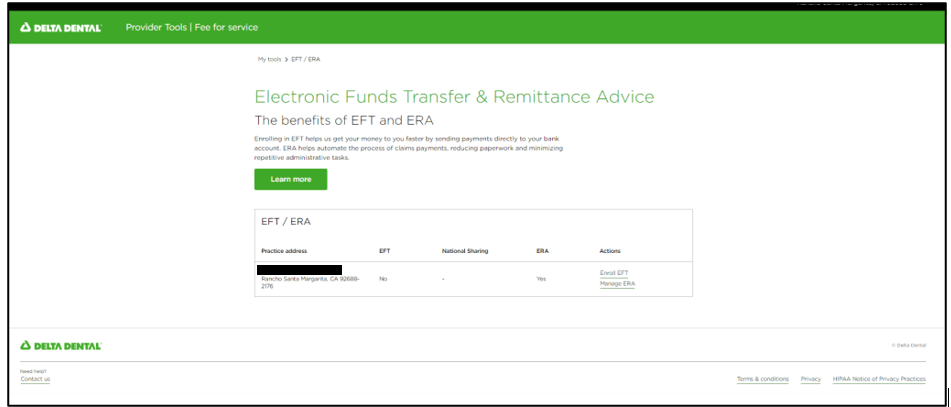
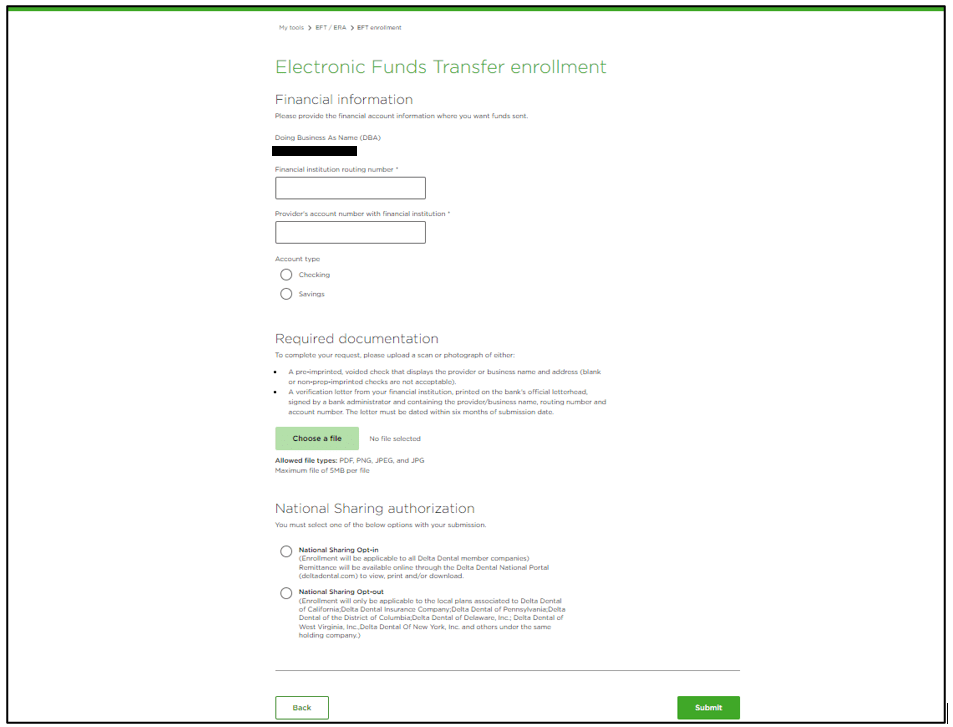
Claim Disputes
Providers who have the unfortunate situation arise when their claim is denied have the option to dispute the decision made by Delta Dental. In the old world, providers had to fill out a paper form and include a paper/photo copy of items such as x-rays or other documents in this form that they had to mail or fax to Delta Dental, which often took weeks to process. By building an online form and keeping the dispute information housed completely within the provider tools platform, providers have improved transparency into their claim decision as well as faster turn around times in adjudicating the decision.
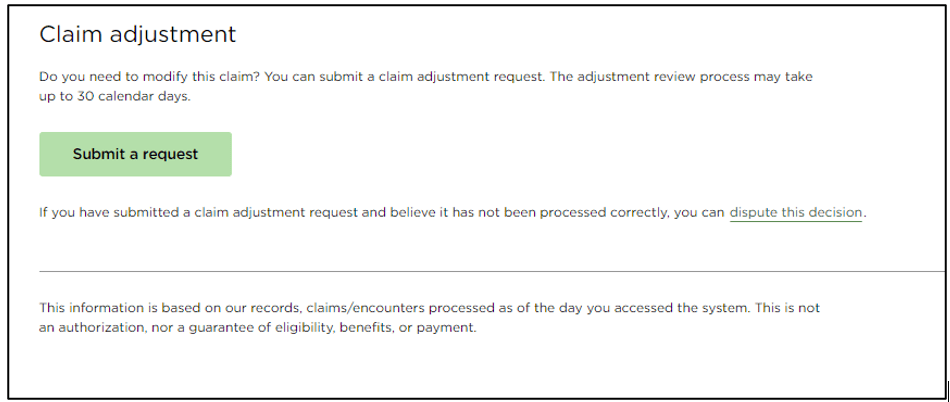
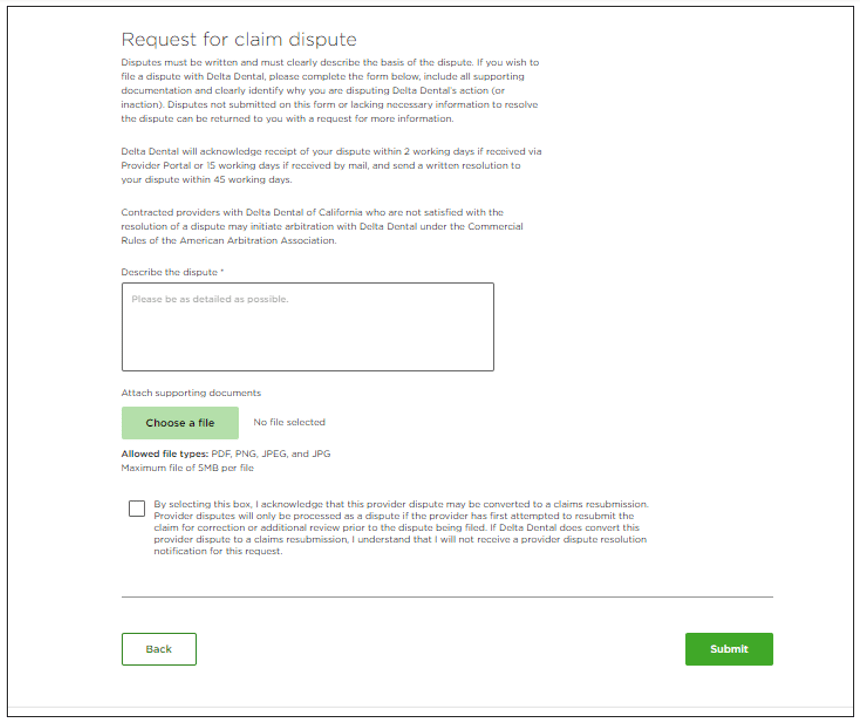
New Contracted Fees
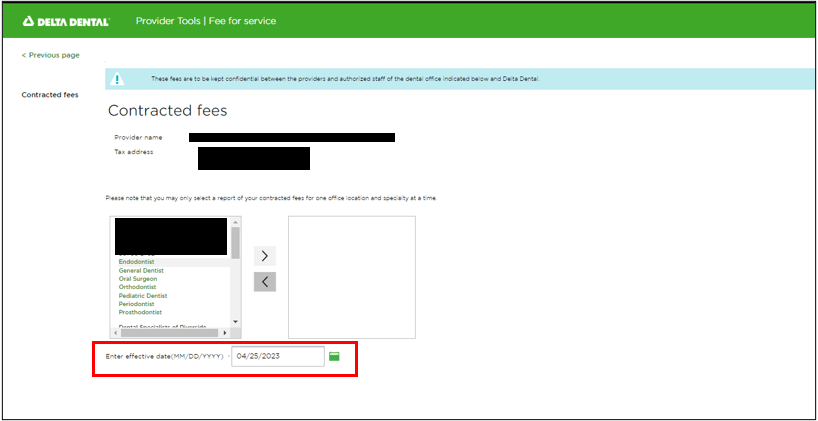
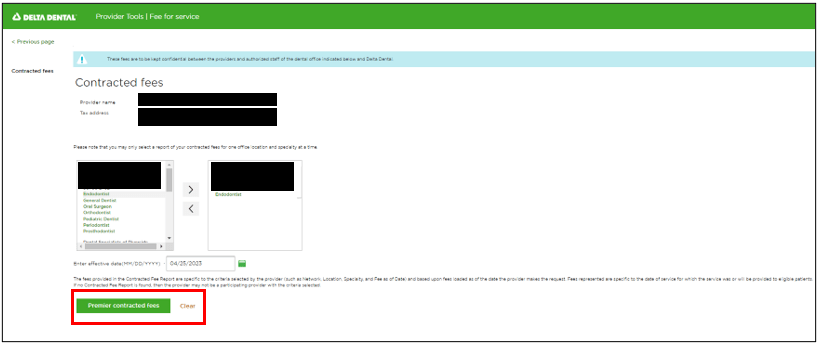
As part of a compliance requirement, California state insurance regulators required more transparency around providing fee schedules for providers based on their specialty (General Dentist, Orthodontist, etc.) and what type of contract they select (PPO or Premier). We built an enhancement in our Provider Tools that allowed for providers to select their office, their service type, and the effective date they wanted to see their fee schedules, which would then generate a report for them to download. This has been part of our mission to provide better trust and transparency with our providers
Updated Claim Submission Flows
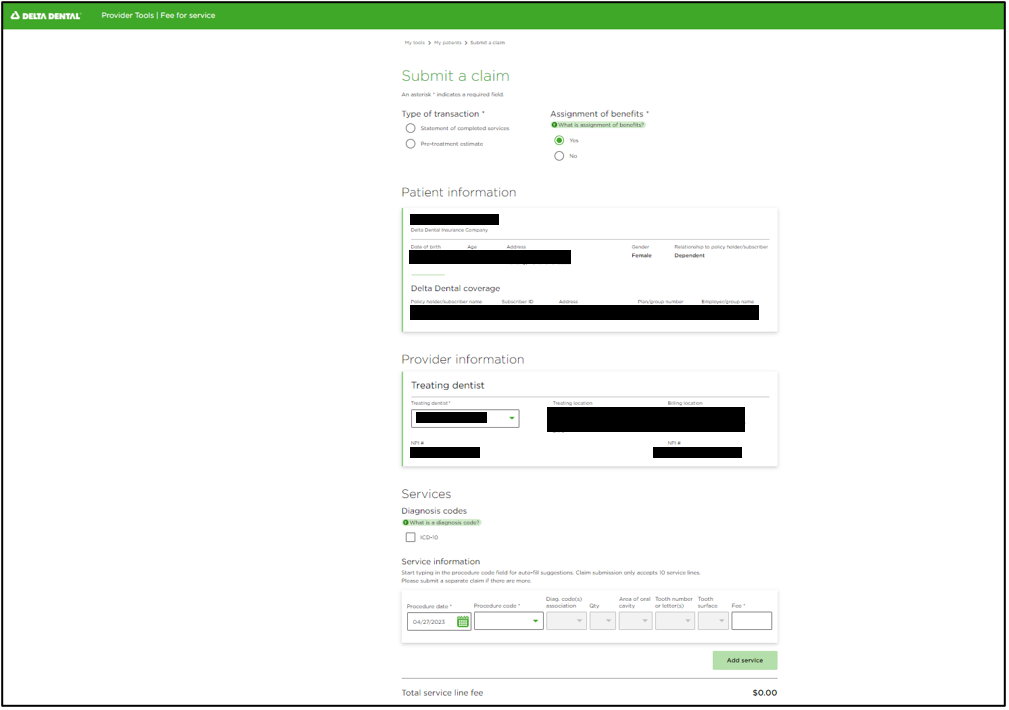
My team was responsible for a new updated Claims feature based on the platform migration from Oracle ADF to a more modernized microservices and React UI based technology. The Claims feature is the largest and most impactful feature to date. By creating a consolidated & clean view of claims and explanation codes as well as create better transparency into the status of the claim, this process will reduce the number of disputes filed as well as inbound calls.
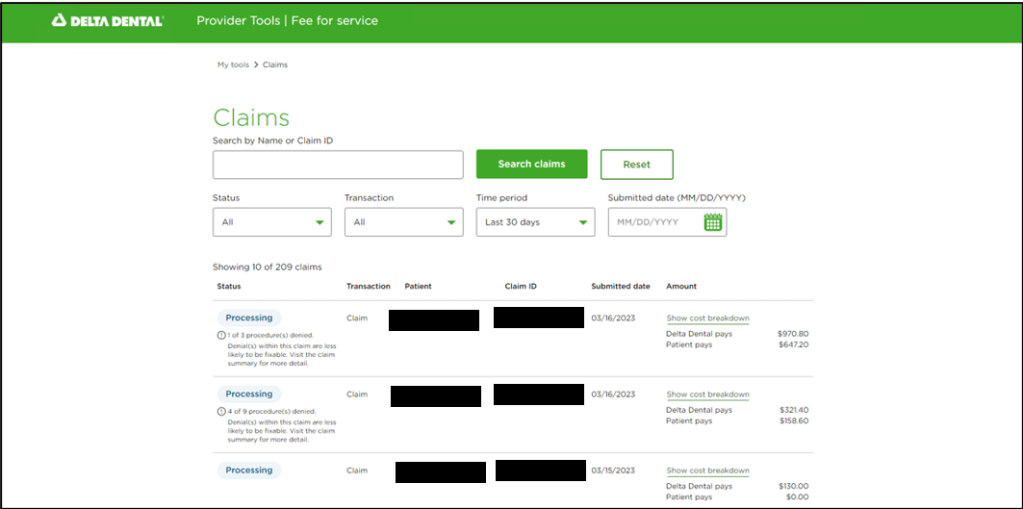
In our first 3 months since its launch, our team has seen over 1M claim submissions within the Provider Tools platform!
Leave a comment